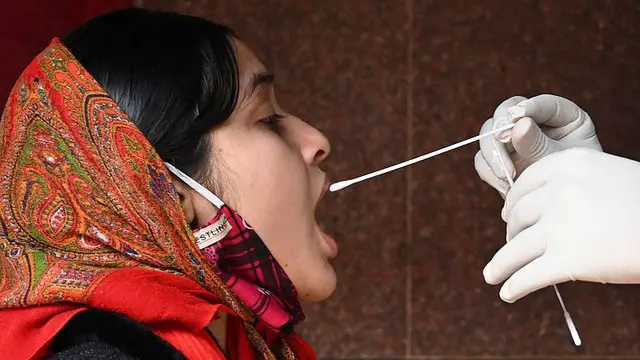
A healthy population is both a cause and a result of economic growth and development. But achieving both today requires policymakers to leave their comfort zones. Specifically, a new generation of global crises – including pandemics, climate change, and increasing hunger – call for a fundamental rethink of finance ministers' role.
We should know. As former finance ministers, we believe that macroeconomic policies now require far greater engagement with line ministries. In particular, finance ministers need to be better able to assess the potential economic effects of public-health risks, introduce taxes that improve health outcomes, and adopt budgetary and regulatory decisions that look beyond short-term public-finance considerations. Failure to do so will mean being unprepared for the next health and economic crisis.
The devastating economic consequences of the COVID-19 pandemic have shown why finance ministers must anticipate their responses to global health risks. The pandemic is forecast to kill more than 15 million people and cost the global economy more than $12 trillion in forgone GDP by 2024. Lockdowns that would have been unimaginable only a few years ago have resulted in more than 1.5 billion students being affected by school and university closures, implying severe long-term consequences for a generation of children and young adults, especially those with no access to effective home schooling.
Simply put, the economic impact of today's systemic health crises may be so large that finance ministers can no longer assume that national and global health policy, especially risk and preparedness assessments for different shocks, is the exclusive domain of health-sector professionals. Instead, finance ministers need to engage more with health leaders to strengthen their countries' resilience in any future crisis.
In many countries, the finance minister has until now set only the overall budgets of line ministries with responsibility for health, leaving implementation to the relevant departments. Similarly, the day-to-day demands on health ministers have often pushed them to focus more on running public-sector hospitals and health-care facilities than on the health of the population, crisis prevention, and response preparedness. These narrow conceptions of their respective roles have led to suboptimal health and economic outcomes.
Finance ministers therefore need to become more directly involved in decision-making in key areas affecting public health and economic performance. A multisectoral approach is essential to identify the policies and budget chapters that have health implications in areas such as water and sanitation, nutrition and sports, clean energy, girls' education, and school-meal programs.
In the past decade, for example, South Africa provided free and tax-free sanitary pads for schoolgirls and women, Chile introduced food labeling and changed school-feeding programs, and Mexico eliminated sugar in milk in daycare centers. As these examples show, the finance-health relationship marks the rhythm, but contributions from other sectors are needed to complete the symphony.
Moreover, value for money should be at the center of public financing of health care. Increased efficiency needs to go hand in hand with greater equity. The discussion must move beyond short-term budgets to joint oversight of the health system's overall efficacy through better procurement, improved financial management, and accountability mechanisms to help ensure that health-care funds achieve specific outcomes sustainably and equitably.
For example, Colombia adopted price controls in its health sector based on data from global markets. Mexico consolidated public-sector medicine purchases and automatically authorized medicines already approved by U.S., European, and Japanese regulators. Argentina introduced an auction system at the national organization to provide care for the elderly cost-effectively. South Africa and India are jointly seeking a waiver from the TRIPS (Trade-Related Aspects of Intellectual Property Rights) agreement regarding the prevention, containment, and treatment of COVID-19 to address market failures, particularly the exorbitant cost of essential public goods like mass vaccination.
Financial concerns aside, formulating the right public policies and regulations is vital to promoting better public health. Here, finance ministers can introduce taxes on unhealthy products; increase research and development spending in health; strengthen competition regulations to hold down pharmaceutical and medical equipment prices; ensure robust rules for public and private health insurers; and contain households' direct out-of-pocket expenditures.
To this end, South Africa, Nigeria, Mexico, and Gabon introduced taxes on sugar-sweetened beverages; Argentina and Colombia hiked tobacco taxes; and Gabon imposed an excise tax on cigarettes. Nigeria instituted a phone tax to fund health-care provision, and South Africa intends to introduce levies on vaping and electronic cigarettes to discourage their use, especially by young people.
Lastly, the COVID-19 pandemic has demonstrated that global health problems cannot be resolved at the national level alone. Reimagining the health-economy dialogue must include rethinking the governance and performance of international financial and health institutions, and bolstering their cooperation. Moreover, these organizations should include health-crisis prevention and response capacity in their macroeconomic risk assessments.
Current global crises demand that health and economic policymakers reinvent and strengthen their collaboration at the national and international levels. By playing a central role in this process, finance ministers can contribute to making a world that is better able to withstand future health-related economic threats.
(CGTN)
 简体中文
简体中文